 “The percentage of patients who get PCO is highly variable and dependent on the type of IOL implanted, surgical technique, cleaning of cortical material, and care in removing lens epithelial cells from the anterior capsule,” notes Dr. 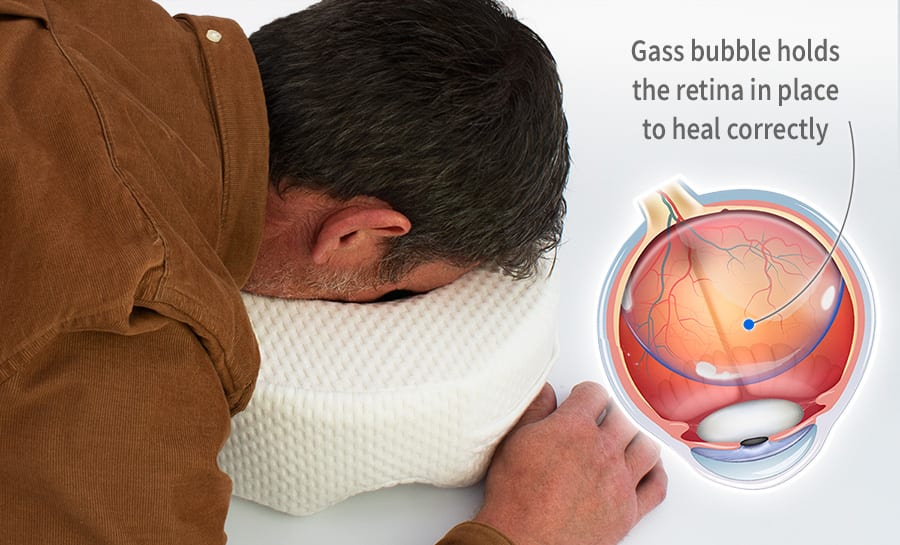
Most surgeons agree, however, that early or later onset is correlated with IOL type, length of follow-up, and whether the cataract surgery was performed in a developing country. Opinions also differ as to the actual incidence of PCO over time. But “the bottom line is we haven’t achieved anything that approaches a good way to eliminate PCO,” Dr. The prevention of PCO through IOL design, and the elimination of proliferating lens epithelial cells with various capsule polishing techniques, chemicals and lasers has been attempted for decades. “Their incidence of retinal tears/detachments just after cataract surgery alone could be 5 percent or higher, and that rate probably increases after posterior capsulotomy,” he says.Īlthough today’s technologies and techniques appear to have decreased the incidence of PCO, they may only have delayed its onset. However, some sub-populations are at more risk-specifically men with high myopia in their 50s and early 60s, says Douglas Koch, MD, professor and chair at the Cullen Eye Institute, Baylor College of Medicine in Dallas. Te is often questioned as being too high,” he notes. Surgeons say to hold off on a posterior YAG capsulotomy for about three months postop just in case a lens exchange is warranted. Among them is Eric Donnenfeld, MD, clinical professor of ophthalmology at New York University. Many surgeons agree the 1 to 2 percent RD rate following Nd:YAG capsulotomy may not be representative of today’s clinical practice. Snyder acknowledges that the YAG procedure is “a cost and an inconvenience, and access to care can be a problem in some rural communities, but it remains a good solution.” “Rather, coincidence with the natural history of retinal detachment plays a bigger role than stresses induced at the time of capsulotomy,” he says. Michael Snyder, MD, associate professor of ophthalmology at the University of Cincinnati, is somewhat skeptical that the YAG causes most RDs after capsulotomy. It’s a life-changing event for the patient who develops one.” 
“Even though our paper shows that the incidence of retinal detachment is lower than what we thought, it’s still not zero. I tell patients the risk is about one in 200 or 0.5%,” he says. Older surgical and YAG capsulotomy techniques and older implant technology may account for the discrepancy between “what the text- books and literature said and what we saw in practice. Rudnisky says that when RD occurs two years post-Nd:YAG it would be hard to prove the YAG caused it. The findings suggest that RD risk is highest in the first five months post-procedure. The incidence of retinal detachment was 0.87 percent at five months post Nd:YAG the rate of retinal tears after Nd:YAG capsulotomy at five months was 0.29 percent. the rate is substantially lower, between 0.5 and 1 percent.” 1 He found the conventionally cited 1 to 2 percent RD rate “overstates the truth. Some were followed out to 10 years (2003 to 2013). Rudnisky evaluated the incidence of RD from an administrative dataset of patients from all age groups who received foldable implants with square edges and were followed-up at 90,120 and 150 days, and then six months and one year post-Nd:YAG capsulotomy. And even though the conventionally accepted incidence of 1 to 2 percent is low, the reality may be much lower, according to research 1 conducted by Christopher Rudnisky, MD, a professor at the University of Alberta in Edmonton, Canada.ĭr. Polishing techniques, chemical treatments and other types of lasers have been tried in the war against PCO.ĭebating the need for a posterior capsulotomy. 
The risk of causing retinal detachment is the first factor cataract surgeons cite when new data, long-term side effects, and the true rate of retinal and other complications. So why are some experts rethinking the risk/benefit ratio of Neodymium:YAG (Nd:YAG) laser capsulotomy for posterior capsule opacification after phacoemulsification and intraocular lens implantation? Controversy swirls around old vs. Cataract surgeons have banked on its efficacy and reliability for decades. By most accounts, it’s one of the most common and trusted procedures in ophthalmology, with a long track record. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
